
Endoscopy
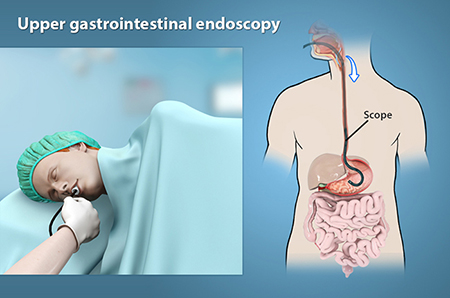
A gastroscopy, also known as an endoscopy is a procedure performed by a doctor, a well-trained subspecialist who uses the endoscope to diagnose and, in some cases, treat problems of the upper digestive system.
The endoscope is a long, thin, flexible tube with a tiny video camera and light on the end.
By adjusting the various controls on the endoscope, the doctor can safely guide the instrument to carefully examine the inside lining of the upper digestive system.
Diagnostic Indications for Endoscopy
- Difficulty in Swallowing
- Persistent isolated nausea or vomiting. In the event of isolated nausea or vomiting persisting for more than 2 days, investigation of the upper gastrointestinal tract is justified after any non-gastrointestinal origin and acute intestinal occlusion have been eliminated
- Digestive disorders. Upper gastrointestinal endoscopy is recommended in
- In subjects aged over 45 years and/or if there are any warning signs or symptom’s such as anaemia, difficulty swallowing, weight loss or any other warning signs and symptoms
- In subjects aged under 45 years with no warning signs or symptoms, upper gastrointestinal endoscopy is recommended in the following situations
- Positive diagnostic test for Helicobacter pylori
- When symptomatic treatment has failed or recurrence occurs at the end of treatment
- Chronic anaemia and/or iron deficiency anaemia. Upper gastrointestinal endoscopy is recommended in iron-deficiency anaemia and/or iron deficiency, after any non-gastrointestinal origin has been eliminated
- Acute gastrointestinal bleeding originating in the upper gastrointestinal tract. Upper gastrointestinal endoscopy is recommended as first choice in acute digestive bleeding which is assumed to originate in the upper gastrointestinal tract (hematemesis or melena)
- Gastro Oesophageal reflux (GORD). Upper gastrointestinal endoscopy is recommended if there are symptoms of gastro oesophageal reflux combined with warning signs (weight loss, dysphagia, bleeding, anaemia), or if the patient is aged over 50 years, or if there is a recurrence on withdrawal of treatment or resistance to medical treatment
Colonoscopy
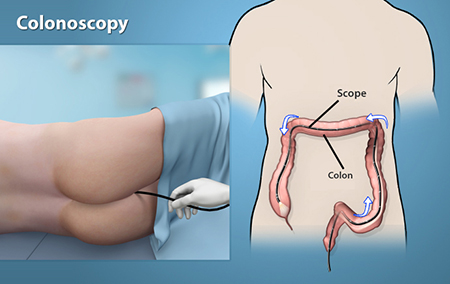
Colonoscopy is a procedure used to view large intestine (colon and rectum) using an instrument called colonoscope (a flexible tube with a small camera and lens attached). The procedure can detect inflamed tissue, ulcers, and abnormal growths. It is used to diagnose early signs of colorectal cancer, bowel disorders, abdominal pain, muscle spasms, inflamed tissue, ulcers, anal bleeding, and non-dietary weight loss.
The procedure is done under general anaesthesia. The colonoscope is inserted into the rectum which gently moves up through the colon until it reaches the cecum (junction of small and large intestine). Colonoscopy provides an instant diagnosis of many conditions of the colon and is more sensitive than X-ray.
The colonoscope is then withdrawn very slowly as the camera shows pictures of the colon and rectum onto a large screen. Polyps or growths can also be removed by colonoscopy which can be sent later for detection of cancer.
Instructions for colonoscopy
Your physician may provide you written instructions and also will be communicate verbally on how to get prepared for the colonoscopy procedure. The process is called bowel preparation.
Gastrointestinal (GI) tract should be devoid of solid food; a strict liquid diet should be followed for 1 to 3 days before the procedure. Patients should not drink beverages containing red or purple dye. Liquids that can be taken before surgery include fruit juices, plain coffee, tea, and water.
Certain medications such as aspirin, ibuprofen, naproxen or other blood thinning medications, iron containing preparation should be stopped before the test. Iron medications produce a dark black stool, and this makes the view inside the bowel less clear.
A laxative or an enema may be required the night before a colonoscopy. Laxative is medicine that loosens stool and increases bowel movements. Laxatives are usually swallowed in pill form or as a powder dissolved in water.
Driving is not permitted for 12 hours after colonoscopy.









